Determiners of pressure ulcers formation – analyses from hospital information system
Determinanty vzniku dekubitů – analýzy z nemocničního informačního systému
Úvod: Proleženiny jsou nežádoucí komplikací během hospitalizace. Cíl: Retrospektivní analýza dat k ověření prevalence dekubitů od roku 2015 (od povinné registrace nežádoucí události dekubitus) dle hlavní diagnózy, typu operace a délky hospitalizace v období 2015–2021. Soubor a metodika: Analýza dat z nemocničního informačního systému (NIS), na hladině významnosti 0,05 (T-Test) s proměnnými: věk, počet proleženin, hlavní diagnóza, operace, délka hospitalizace a výskyt COVID-19 k délce hospitalizace. Výsledky: Celkem bylo v NIS evidováno 2 350 dekubitů u 1 539 nemocných (1,52 dekubitu/pacienta) a 930 (40 %) nemocných bylo přijato k hospitalizaci s dekubity. Nejčastější lokalizace dekubitů: pata (33 %), sakrum o 6 % méně, hýždě (17 %). V letech 2015–2021 bylo operováno 17 247 nemocných, z nich 289 nemocných mělo dekubitus. Nejčastější hlavní diagnóza při výskytu dekubitů byla fraktura krčku kosti stehenní (14,35 %) a neurologické (9,09 %) či onkologické onemocnění (12,03 %). Překvapivý byl výskyt dekubitů u nemocných s ileózními stavy (11,57 %). COVID-19 byl v letech 2020 a 2021 zjištěn u 163 pacientů, z nichž šest mělo dekubitus a prodlouženou hospitalizaci. Závěr: Zdravotní stav osob s chronickými ranami i dekubity je důležité vnímat komplexně a individuální plán péče vypracovat s cílem zlepšit život pacientů a šanci na uzdravení.
Klíčová slova:
dekubity – COVID-19 – délka hospitalizace – proleženiny – chirurgická infekce
Authors:
L. Veverková 1
; P. Doležal 2; M. Reška 1; P. Vlček 1; L. Urbánek 1; J. Habr 1; I. Penka 1
Authors‘ workplace:
1st Surgical Department, Faculty, of Medicine, Masaryk University, and St. Anne University Hospital, of Brno, Brno
1; Consulting s. r. o. cz, Brno
2
Published in:
Cesk Slov Neurol N 2022; 85(Supplementum 1): 52-56
doi:
https://doi.org/10.48095/cccsnn2022S52
Overview
Introductions: Pressure ulcers (PUs) represents an undesirable complication during hospitalization. Aim: Retrospective data analysis to verify the prevalence of PUs since 2015 (since the mandatory registration of the PUs an adverse event) by principal diagnosis, type of surgery and length of hospital stay in the period 2015–2021. Sample and methods: Retrospective analysis of data from the hospital information system (HIS), at 0.05 level of significance (T-Test) with the variables: age, number of pressure ulcers, principal diagnosis, operation, length of hospitalization and prevalence of COVID-19 to length of hospitalization. Results: A total of 2,350 PU cases in 1,539 patients (1.52 PUs/patient) were registered in the HIS, and 930 (40%) patients were admitted to hospital with PUs. The most common locations of PUs were: heel (33%), sacrum 6% less, buttocks (17%). Between 2015 and 2021; 17,247 patients were operated on, of whom 289 had a Pus. The most common principal diagnosis in the occurrence of PUS was femoral neck fracture (14.35%) and neurological (9.09%) or oncological disease (12.03%). The incidence of PUs was surprising in patients with ileal conditions (11.57%). COVID-19 was found in 163 patients in 2020 and 2021, six of whom had PUs and prolonged hospitalization. Conclusion: It is important to view the health status of people with chronic wounds and PUs in a comprehensive manner and to develop an individualized care plan to improve patients‘ lives and chances of recovery.
Keywords:
pressure ulcers – pressure sore – COVID-19 – surgical infection – length of hospitalization
Introduction
The skin represents the main barrier against microbial invasion. Intact and well-vascularized skin is highly resistant to bacterial invasion [1]. In case of compromised integrity of the skin, an infection will certainly develop at the site of damage. Infections developing in damaged skin represent a diverse group of wounds, including pressure ulcers (PUs) [2].
Pressure ulcers (bedsores and pressure injuries) are localized areas of tissue necrosis arising from prolonged compression of soft tissues between the bone spur and the outer surface. They pose a serious problem in critically ill patients, older adults and people with injuries and represent one of the most common types of complicated wounds. Each open PUs is superficially contaminated with the flora from the environment. However, it is important to prevent further contamination in case the wound is located near the anal opening, as is the case with ischial or sacral pressure ulcers. Infections of the skin and soft tissues include a variety of pathologies that affect the skin and subcutaneous tissue, fascia or muscle, ranging from simple superficial infections to severe necrotizing infections that require surgical intervention with drainage and debridement followed by long-term treatment [3]. Standard care for adults with PUs includes proper prevention and treatment. Each occurrence of PUs must be reported as adverse events in the system – this is a mandatory obligation applying to all inpatient care providers in the Czech Republic [4].
Material and methods
We used data generated by the hospital information system (HIS). The statistical analysis was performed using T-Test at significance level of 0.05. The variables used included: age, number, category of PUs and main diagnosis, surgery, duration of hospitalization and the information whether the incidence of COVID-19 affected the length of stay in patients with Pus.
Results
Throughout the period from 2015 to December 31, 2021, the entire St. Anne‘s University Hospital of Brno; 2,350 PUs were recorded in the hospital information system. This figure represents the number of cases – i.e., all localizations even of multiple PUs and it account for 0.95% out of the total number of hospitalized patients. The development in individual years is described in Tab. 1 and Fig. 1 that show a visible decrease in the incidence of this undesirable event, respectively infection in the wound following a change in approach and introduction of consistent prevention of PUS and the start of the obligation to regularly report this adverse event.
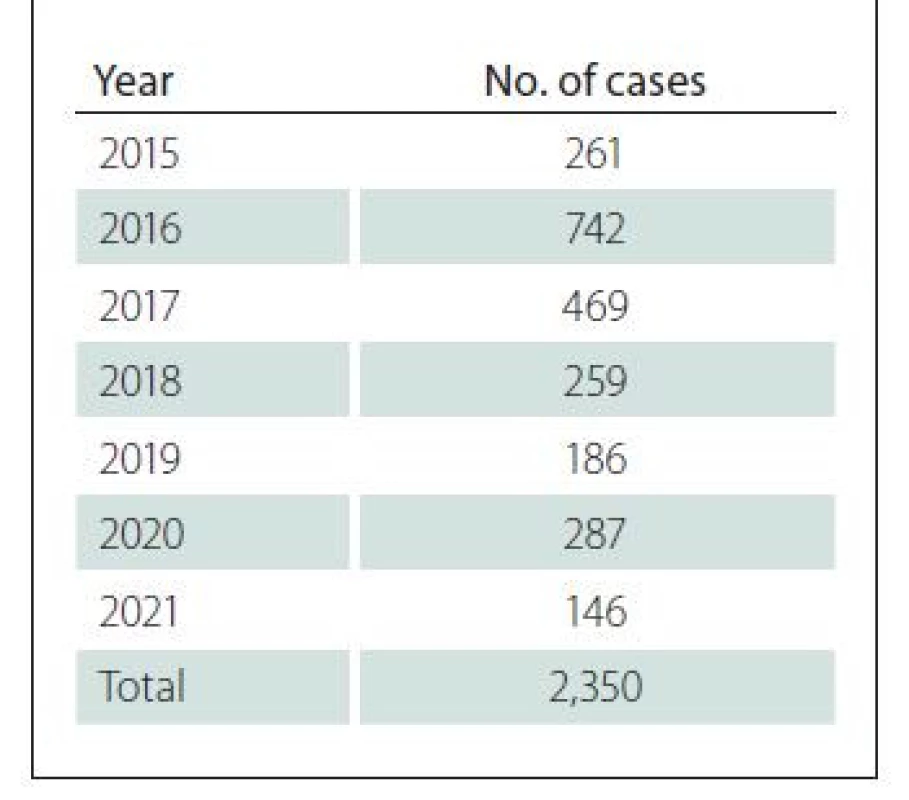
Obr. 1. Počet dekubitů v průběhu let.

The age of the patients represents a predictive factor in the development of the PUS. Within our entire group of 1,539 patients with PUs, this corresponds to the median age of 80 years. There were 1.52 PUs per patient. The Fig. 1 shows a clear trend of declining incidence of PUs throughout the hospital until 2020, when there was a temporary increase caused by the COVID-19 pandemic.
The database showed a difference between the age of men and women with developed PUs. The average age of patients with PUs was 77.12 years. In the male group, the age was 75.11 years, and in women it was 78.86 years (Tab. 2, Fig. 2). Women with PUS were 3 years older than men. This difference is statistically significant (P-value = 2.082E-07).
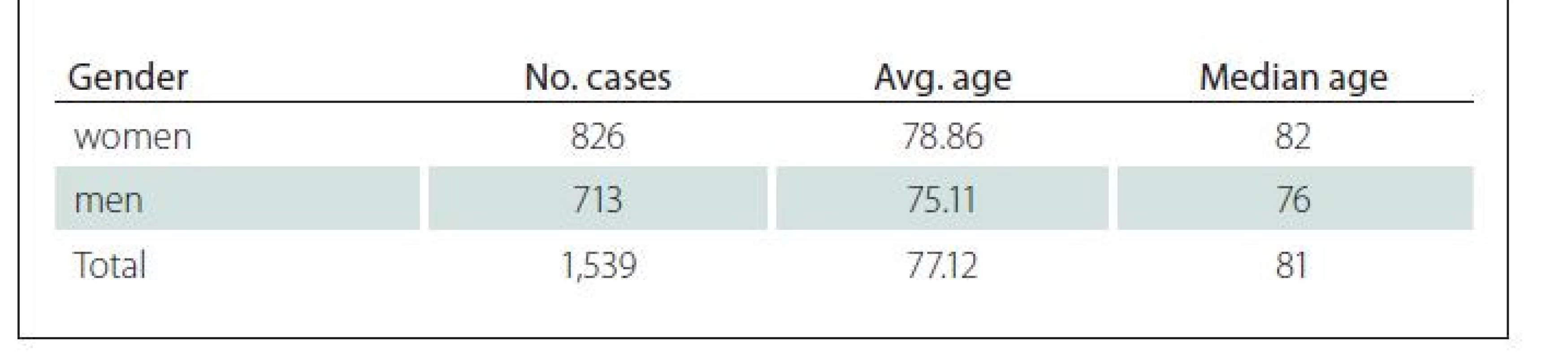
Obr. 2. Počet případů dekubitů podle věku.

An interesting finding was the place where the PUs developed and its localization. In total, 930 documented PUs developed outside the hospital, i.e., patients were admitted to hospital already with developed PUs. This number accounts for almost 40% of all patients in our group. Remaining PUs developed during the stay in hospital (Tab. 3).
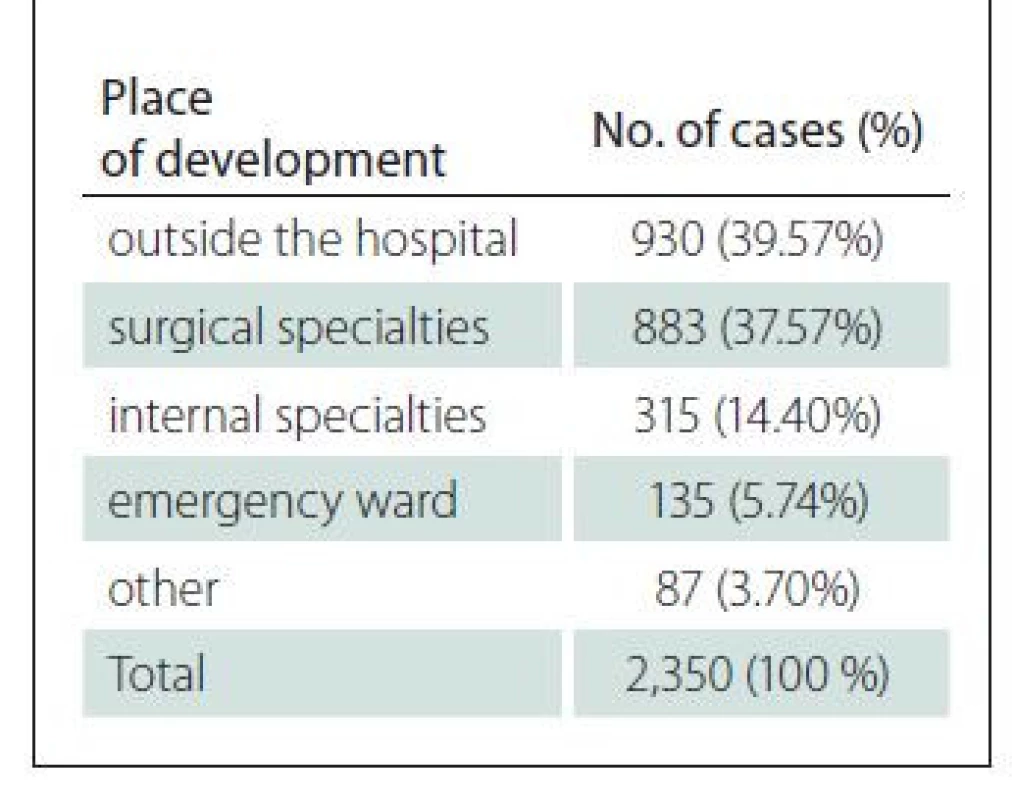
Despite the high number of patients recorded in the surgical ward, only 432 patients with PUs were operated.
The most typical were patients with PUs on heels. This group accounted for 773 patients – almost 33%. Number of patients with PUs in the sacral area six percentage points lower – only 27% of the total number of all the registered PUs. The third most common area affected by a PUs was the buttocks, which represented 17% of the total number of cases (Tab. 4).
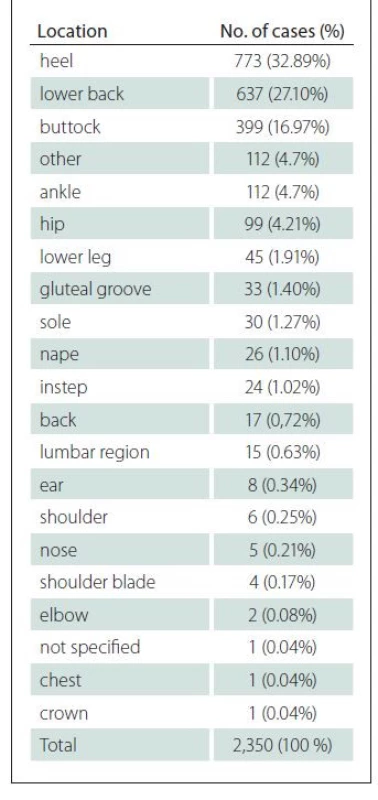
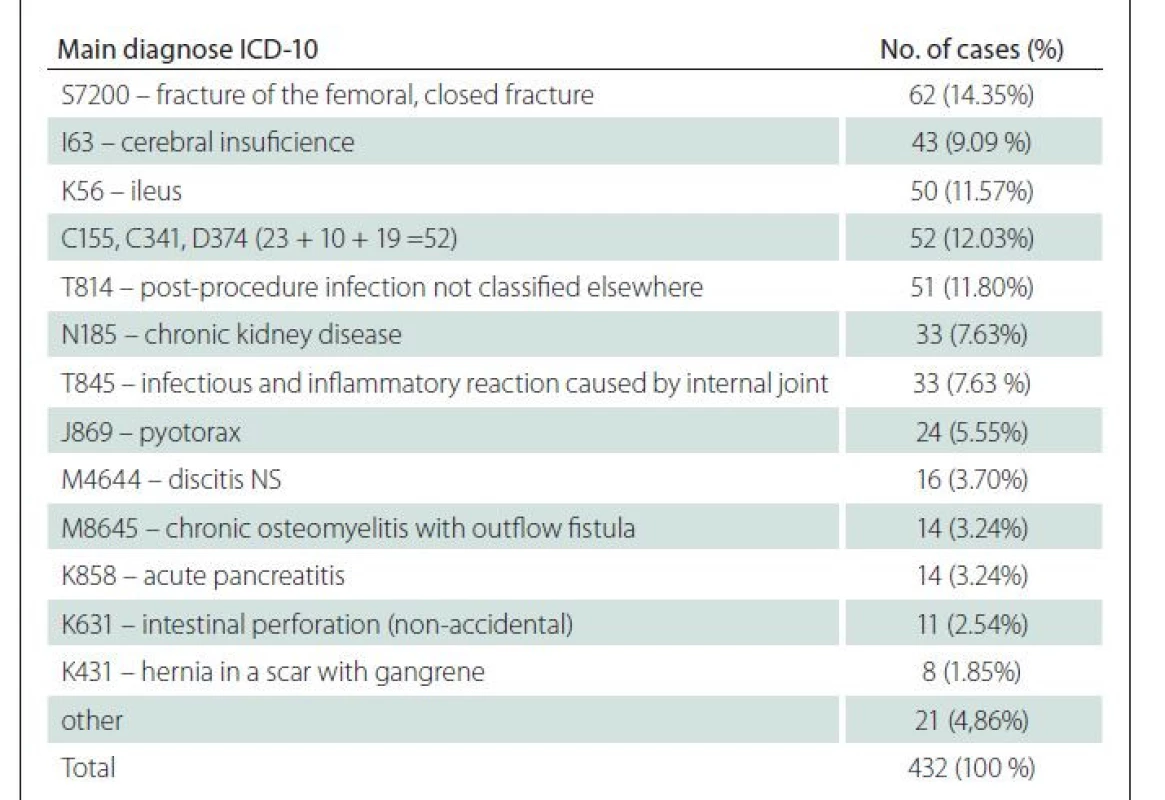
At the 1st Surgical Clinic, a total of 17,247 patients were operated on in the reviewed period between 2015 and 2021. Of these, 289 patients developed a PUs. Most commonly, the PUs developed in patients with the femoral neck fracture (dg. S72 according the ICD-10), which accounts for 17.41% of all PUs throughout the reviewed period (Tab. 5). One of the key factors in the development of PUs is neurological and oncological diseases. We have demonstrated this in previous studies and the results were published in 2019 [5]. In the current study, this fact has been confirmed again. Brain disease occurred in 62 patients – 21.45% of all cases, and an oncological diagnosis was the main factor in 52 – 17.99% of all cases. A complete surprise was the finding of the development of PUs in patients whose main diagnosis was ileus and who’s accounted for 17.30% of all cases.
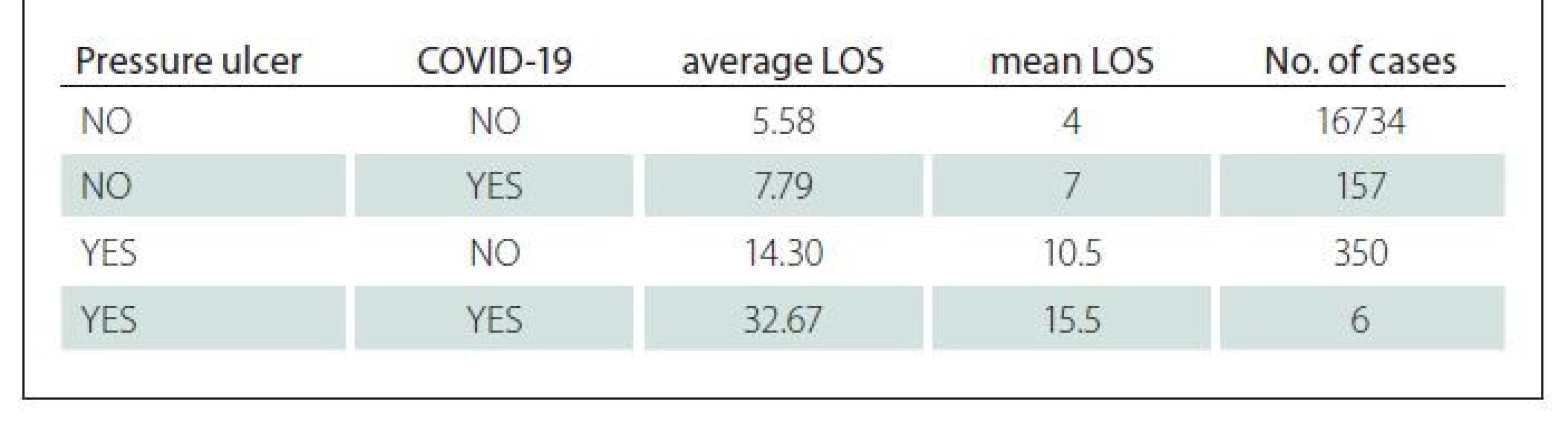
COVID-19 in 2020 and 2021 was diagnosed in 163 patients of whom six also suffered from Pus. The period of hospitalization represents an important aspect in the assessment of the clinical ward, but also works as a financial tool used by the insurance companies and reimbursement. The average length of stay in all patients amounted 5.58 days, the mean value was 4 days. In case the patient developed a PUs, the length of stay extended to 14.30 days and this is statistically significant (P-value = 6,2549E-24). In patients with combination of a PUs and COVID-19, the length of stay climbed to 32.67 days, which represents an extension of 585%. But this is not statistically significant (P-value = 0.1496). The difference in the mean values, including percentiles and mean hospital stay (5.8 days for patients without PUs and COVID-19 and 32.67 for patients with COVID-19 and PUs) is significant and indicates a statistical relationship between the incidence of PUs and COVID-19. Welch‘s T-test does not support this hypothesis. The reason for this is the disproportion in the samples – about 17,000 vs. six cases and the large number of outliers in the larger sample. In the case of an increase in the number of patients with PUs ulcers and COVID-19 positivity, it is possible and probably likely that not a larger sample of these patients will confirm the hypothesis (Fig. 3, Tab. 6).
Obr. 3. Statistické závislosti mezi pacienty s dekubity a s infekcí COVID-19 a bez infekce.

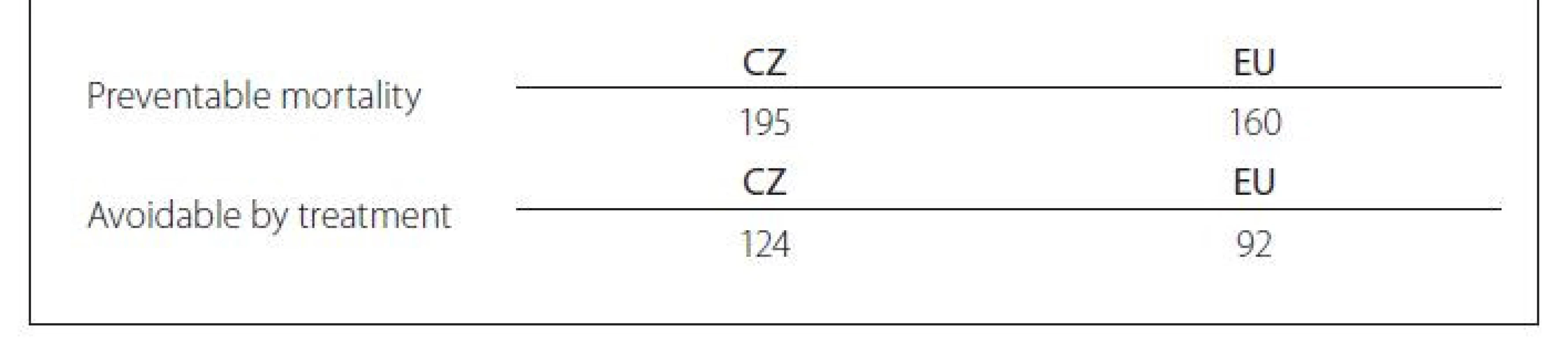
In the monitored period, the death rate at our clinic reached 12.65%, but in the years of the COVID-19 pandemic the percentage of deaths increased more than twice to 27.36%. In Tab. 7 you can see Age-standardized mortality per 100,000 inhabitants in the Czech Republic and European Union (EU).

Discussion
Although the Czech Republic spends significantly less on its healthcare than most other EU countries, its healthcare system provides a wide range of reimbursed health services. Demographic factors in our country are known and the population size is 10,693,939, of which the share of the population older than 65 years of age accounts for 19.9%, which is in contrast with other EU states. Life expectancy in the Czech Republic has been steadily increasing in the last 10 years, but in 2019 it was 79.3 years, which is two years lower than the EU average [6]. Unlike in other EU countries, the proportion of remaining years that a citizen of the Czech Republic may live without disability increases with increasing age. Despite a certain progress achieved in the last decade, the Czech Republic before the pandemic still had a high mortality rate from preventable and treatable causes. The so-called „preventable mortality“ per 100,000 inhabitants in the Czech Republic is higher than in other EU countries – in 2018 the number was 195 in the Czech Republic compared to 160 in the EU, and development of pressure ulcers represents one of the causes of death [7].
Necrotizing infections of soft tissues, where also PUs of especially categories 3 and 4 belong, represent a potentially life-threatening and debilitating infection with approximately 20–30% of patients dying during a hospital stay [1].
In our group of patients monitored over the period of 7 years, we have shown that at least 40% of patients were admitted to the hospital already with PUs that developed in another environment, which is lower than the literature data published by the Institute of Health Information and Statistics of the Czech Republic. The most common location of PUs in our group was the heel. In relation to the main diagnosis, the percentage of PUs was in 17.41% of patients with a femoral neck fracture, but of the total number of patients operated on with this diagnosis in the seven-year reviewed period, this diagnoses accounts only for 1.32% of cases. Brain diseases and oncological diseases occurred in more than 10% of cases. But an absolutely surprising finding was the occurrence of PUs in patients with an ileus condition.
Preventive measures that were introduced throughout the hospital clearly led to a decrease in the incidence of PUs throughout the hospital. This good development trend was disrupted by the global COVID-19 pandemic, which resulted in extended length of stay in patients with PUs, which was statistically significant, nevertheless there was also an increased number of deaths throughout the Czech Republic [8].
In 1948, the World Health Organization defined health as „a state of complete physical, mental, and social well-being, and not merely the absence of disease or defect.“ Since then, this definition has not changed. The definition applies as much to people with chronic wounds as it is to people with chronic injuries as well as to the general population.
Conclusion
Globally, the burden of chronic diseases is increasing, with significant differences between countries, age groups and socio-economic status. Pressure ulcers represent a frequent problem especially in frail elderly patients with chronic co-morbidities. The state of health of European Union citizens has been summarised by the Organisation for Economic Co-operation and Development (OECD) in its latest health report, Health at a Glance. It is important to understand the comprehensive health status of people with chronic wounds or those who are at risk of wounds in order to develop interventions for prevention and treatment with the aim to improve the lives of people affected by wounds. Our retrospective analysis has shown us which options can be improved.
Conflict of interest
The authors hereby declare that they have no potential conflicts of interest concerning drugs, products, or services used in the study.
The Editorial Board declares that the manuscript met the ICMJE „Uniform Requirements“ for biomedical papers.
Redakční rada potvrzuje, že rukopis práce splnil ICMJE kritéria pro publikace zasílané do biomedicínských časopisů.
The Editorial Board declares that the manuscript met the ICMJE “uniform requirements” for biomedical papers.
Assoc. Prof. Lenka Veverková, PhD
1st Surgical Department
Faculty of Medical, Masaryk
University
St. Anne University Hospital
Pekařská 53
602 00 Brno
e-mail: lvever@med.muni.cz
Sources
1. Sartelli M, Guirao X, Hardcastle TC et al. 2018 WSES/SIS-E consensus conference: recommendations for the management of skin and soft-tissue infections. World J Emerg Surg 2018; 13 : 58. doi: 10.1186/s13017-018-0219-9.
2. Esposito S, Bassetti M, Borrè S et al. Diagnosis and management of skin and soft-tissue infections (SSTI): a literature review and consensus statement on behalf of the Italian Society of Infectious Diseases and International Society of Chemotherapy. J Chemother 2011; 23 (5): 251–262. doi: 10.1179/joc.2011.23.5.251.
3. Eron LJ, Lipsky BA, Low DE et al. Expert panel on managing skin and soft tissue infections. Managing skin and soft tissue infections: expert panel recommendations on key decision points. J Antimicrob Chemother 2003; 52 (Suppl 1): i3–i17. doi: 10.1093/jac/dkg466.
4. Pokorná A, Benešová K, Mužík J et al. Data Sources for Monitoring of Non-healing Wounds in a National Health Information System – Epidemiology of Non-healing Wounds – Analysis of the National Register of Hospitalized Patients in 2007–2015. Cesk Slov Neurol N 2017; 80/113 (Supp1 1): S8–S17. doi: 10.14735/amcsnn2017S8.
5. Veverková L, Reška M, Vlček P et al. Key factors for the development of pressure ulcers in surgical practice. Cesk Slov Neurol N 2019; 82/115 (Supp1 1): S60–S65. doi: 10.14735/amcsnn2019S60.
6. Alexa J, Rečka L, Votápková J et al. Czech Republic: health system review. Health Syst Transit 2015; 17 (1): 1–165.
7. OECD/EU. Health at a glance: Europe 2020 – state of health in the EU cycle. Paris: OECD Publishing 2020. doi: org/ 10.1787/ 82129230-en.
8. WHO Regional Office for Europe, European Commission, COVID-19 Health Systems Response Monitor – Czech Republic. European Observatory on Health Systems and Policies. 2021 [online]. Available from URL: https: / / eurohealthobservatory.who.int/ monitors/ hsrm/ overview.
Labels
Paediatric neurology Neurosurgery NeurologyArticle was published in
Czech and Slovak Neurology and Neurosurgery

-
All articles in this issue
- Monitoring the prevalence of pressure ulcers – a comparison of national data with data of a specific health care provider – University Hospital Ostrava
- The use of incontinence devices and urinary/ faecal diversion management devices in hospitalised patients as a possible cause of unwanted immobilization
- Standardization of wound care for patients in Austria, Germany and Slovakia
- Skin grafting in surgical treatment of pressure ulcers
- The use of negative pressure wound therapy in a selected medical facility
- Can different type of the pressure ulcers debridement affect oxidative stress parameters?
- Nurses‘ knowledge in the field of specific prevention and treatment of heels pressure injuries
- Identification of barriers and benefits of Negative Pressure Wound Therapy
- Determiners of pressure ulcers formation – analyses from hospital information system
- Advanced practice nursing in the field of wound management
- Czech and Slovak Neurology and Neurosurgery
- Journal archive
- Current issue
- About the journal
Most read in this issue
- Monitoring the prevalence of pressure ulcers – a comparison of national data with data of a specific health care provider – University Hospital Ostrava
- Nurses‘ knowledge in the field of specific prevention and treatment of heels pressure injuries
- Standardization of wound care for patients in Austria, Germany and Slovakia
- Advanced practice nursing in the field of wound management
