International Cooperation in Pressure Ulcers Prevalence, Prevention and Treatment is Challenged by the Lack of National Registries
Mezinárodní spolupráce v oblasti prevence a léčby dekubitů jako výzva s ohledem na nedostatek národních registrů
Cíl:
Cílem studie bylo analyzovat výsledky mezinárodního průzkumu zaměřeného na proces hodnocení prevalence, prevence a sledování pacientů s dekubity. Snahou bylo zjistit, zda data sledovaná na národní úrovni lze využít pro mezinárodní srovnávání.
Metodika a soubor:
Multicentrická deskriptivní mezinárodní studie orientovaná na zjištění prevalence, prevence a sledování pacientů s dekubity mezi zástupci mezinárodních společností zaměřených na péči o rány a dekubity (Evropské společnosti pro léčbu ran (EWMA) a Evropského poradního panelu pro otázky dekubitů (EPUAP)).
Výsledky:
V průzkumu odpovědělo 16 % z oslovených zemí spolupracujících s EWMA a 10 % kontaktních osob. Ze spolupracujících zemí s EPUAP odpovědělo 71 % zemí a 47 % kontaktních osob.
Závěr:
Většina respondentů odpověděla, že nemají národní registr pro sledování dekubitů, ale na lokální úrovni sledují obdobná data. Nedostatek strukturovaně sledovaných údajů na národní úrovni ovlivňuje možnosti využití dat také na mezinárodní úrovni. Protože stávající data z dosavadních zdrojů v oblasti managementu dekubitů jsou omezená a nekonzistentní, je vhodné zavedení společných minimálních údajů, které by měly být sledovány na mezinárodní úrovni.
Klíčová slova:
pressure ulcers – structured wound management – national quality registries – international cooperation – international survey
Autoři deklarují, že v souvislosti s předmětem studie nemají žádné komerční zájmy.
Redakční rada potvrzuje, že rukopis práce splnil ICMJE kritéria pro publikace zasílané do biomedicínských časopisů.
Authors:
A. Pokorná 1; R. F. Öien 2; H. Forssell 2; C. Lindholm 3
Authors place of work:
Department of Nursing, Faculty of Medicine, Masaryk University, Brno, Czech Republic
1; Blekinge Center of Competence, Karlskrona, Sweden
2; Sophiahemmet University, Stockholm, Sweden
3
Published in the journal:
Cesk Slov Neurol N 2016; 79/112(Supplementum1): 20-24
Category:
Původní práce
doi:
https://doi.org/10.14735/amcsnn2016S20
Summary
Aim:
The aim of this study was to analyse the results from an international survey on prevalence, prevention, and follow-up of patients with pressure ulcers, with a focus on exploring whether a common minimum data set from national quality registries could be used in an international setting.
Material and methods:
A cross-sectional descriptive survey design was used to obtain data from national PU registries. A questionnaire based on a previously performed review of relevant literature was sent to national experts in the field of wound management (European Wound Management Association; EWMA and European Pressure Ulcer Advisory Panel; EPUAP representatives).
Results:
The response rates to the international survey were 16% (countries) and 10% (contact persons) within EWMA and 71% (countries) and 47% (contact persons) within EPUAP.
Conclusion:
The majority of respondents stated that they did not have national registries for PU, but that they registered similar data on a local level. A lack of national data seriously impairs efforts to develop an international research network on patients with PU and to share data and expert knowledge and skills. Although existing data from registries or administrative health records on pressure ulcer management are scarce and inconsistent, the task of establishing a common minimum data set in an international setting seems worthwhile.
Key words:
dekubity – strukturovaná péče o rány – národní registry – mezinárodní spolupráce – mezinárodní průzkum
Introduction
Pressure ulcers (PU), also known as pressure sores or pressure injuries, are usually regarded as avoidable damage to a patient caused by health care [1,2]. They affect a large number of people and result in considerable health system expenditure [3]. Globally, the economic impact of PU has yet to be established, but the estimated cost for their prevention in the U.S. is .66 per day, while the care of a patient with a stage II PU is approximately ,770.54 per day and that of a patient with an unstageable PU (one which cannot be clearly classified) increases to ,622.98 per day [4]. PU belong to a larger group of hard-to-heal ulcers, which can be covered by national registries like the Swedish National Quality Registry of Ulcer Treatment [5]. Another aspect of PU is reduced quality of life, where pain has the strongest impact [6,7].
PU can affect any patient from a new-born child to a patient in palliative care. However, the majority of these patients are older, with different co-morbidities, and they are often treated for long periods of time due to the absence of structure in wound management [5,8,9]. Furthermore, patients with PU are treated by different caregivers, such as community care, hospital care, emergency care, primary health care, and private health care providers, as well as by different medical specialties, which may result in a lack of continuity of care. Patients with hard-to-heal ulcers and PU in particular are considered to belong to a neglected and low-priority medical group, due to the low medical status of ulcer treatment [5,8]. In order to address the complex clinical picture of prevalence, prevention, and follow-up of patients with PU, international cooperation using existing national data and results seems a worthwhile research effort.
Aim
The aim of this study was to analyse the results from an international survey on prevalence, prevention, and follow-up of patients with PU, with a focus on exploring whether a common minimum data set from national quality registries could be used in an international setting.
Methods
International survey
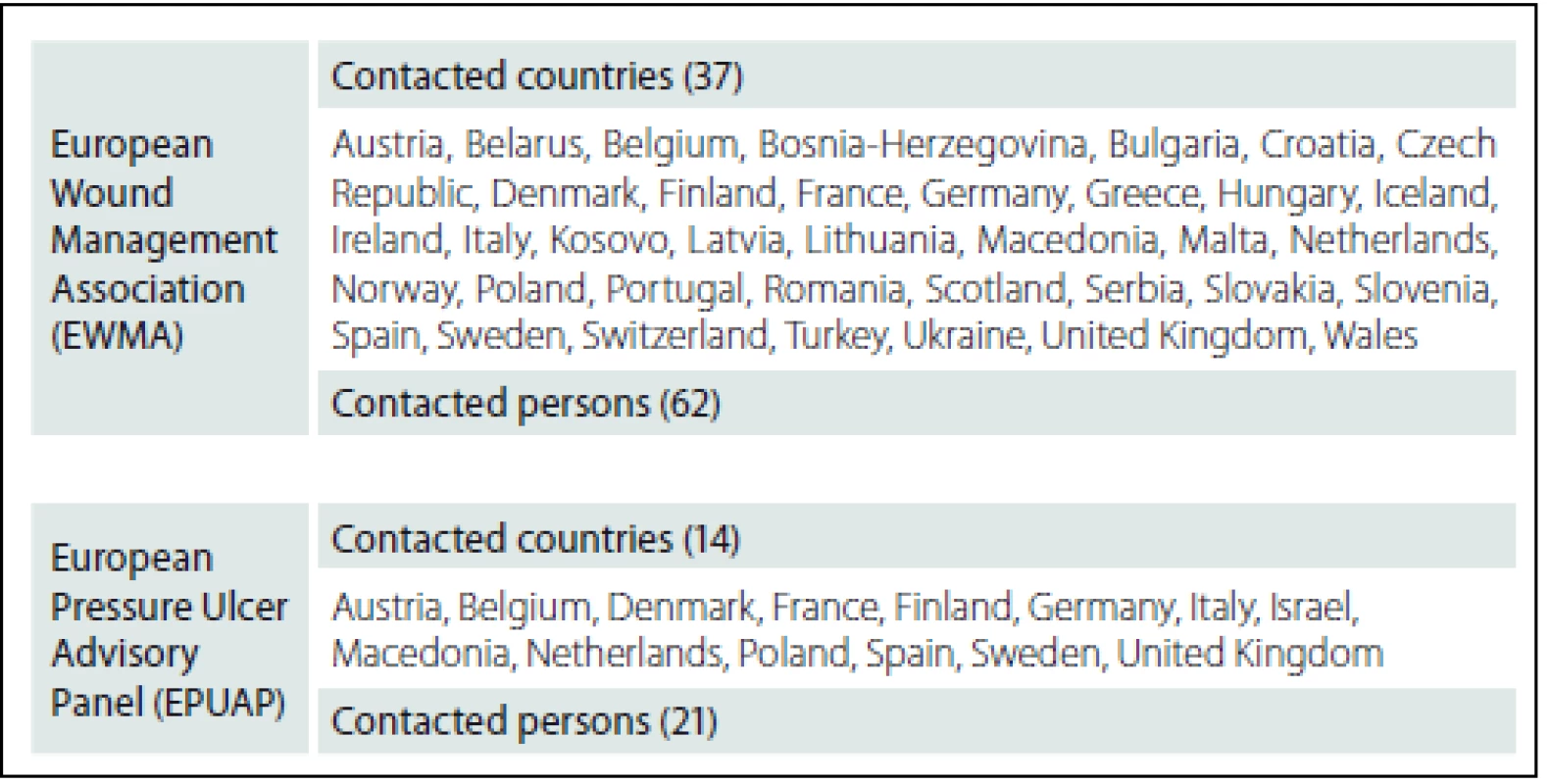
A cross-sectional descriptive survey design was used to obtain data from national PU registries. A questionnaire based on a previously performed review of relevant literature was sent to national experts in the field of wound management. The focus of the questionnaire was ulcer size and location, risk assessment, prevention, treatment, and research results. Invitations to participate were sent in May 2015 to 83 contact persons representing two cooperating organisations covering 52 European countries: the European Wound Management Association (EWMA) and the European Pressure Ulcer Advisory Panel (EPUAP) (tab. 1).
Reminders were sent in July 2015 and September 2015 in collaboration with the EWMA and EPUAP secretariats. The questionnaire was designed and distributed online via email.
The survey was part of a research project on PU within the Czech Republic with the aim of collecting information about existing national quality registries on hard-to-heal ulcers with a special focus on PU. Results from the survey were intended to be used to describe the effect of PU on health-related quality of life (pain in particular) and to develop specific clinical practice guidelines covering all aspects of PU including nutrition, prevalence, prevention, treatment, and follow-up to ulcer healing. The main aim of the Czech project is a newly-created nationwide registry for monitoring of PU at the national level in a structured and uniform manner for inpatient care settings.
There is an ongoing international collaboration and an existing network of researchers, clinicians, and registry developers where data from the Swedish National Quality Registry of Ulcer Treatment (RUT) are requested, and hence this study was carried out in collaboration with RUT.
The Swedish National Quality Registry of Ulcer Treatment
In recent decades, a system of national quality registries has been established in the Swedish health and medical services covering different areas of medicine. The aim of the registries is to gather data on diagnoses, symptoms, interventions, and treatment outcomes in order to give a continuous systematic evaluation of medical practice.
There are currently around 100 registries in Sweden, each of which receives central funding after annual applications to the Swedish Association of Local Authorities and Regions (http:/ / www.skl.se; SKL). The majority of the Swedish national quality registries were developed by physicians with special interest in a research field, in order to bring about quality improvement in healthcare for a specific medical problem. RUT was initiated and developed by a general practitioner (RFÖ, one of the authors of this study) to ensure that patients with hard-to-heal ulcers receive adequate diagnosis and treatment with continuity of care until ulcer healing. It was established in 2009, and today covers more than 5,800 patients nationwide, allowing the provision of reliable statistical data. The registry is web-based, and units can register free of charge. It covers patients with hard-to-heal ulcers, including PU, treated by primary care, community care, homecare, hospitals, and private caregivers.
In 2016, RUT will be interconnected with Senior Alert, a registry covering PU prevention in order to follow patients with PU from prevention (Senior Alert) through treatment to healing (RUT). We will then have the opportunity to illustrate the whole situation for PU patients, including which preventive measures will benefit both the patients and the health care sector. In the light of this perspective, the minimum data set from RUT could be used in an international setting to shed further light on PU in Europe.
Statistical analyses of data from RUT
Statistical analyses were performed using version 14 of the STATA software package (StataCorp LP, College Station, Texas, USA). Continuous variables are expressed as mean values, ranges, and standard deviations (SD), while qualitative variables are presented as numbers and percentages. Healing time was assessed with Kaplan-Meier analysis. A log-rank test was used for evaluation of healing times.
Results
International survey
The response rates to the international survey were 16% (countries) and 10% (contact persons) within EWMA and 71% (countries) and 47% (contact persons) within EPUAP (tab. 2). Two additional countries (Australia and USA) answered after having been contacted by the secretariats of EPUAP and the US National Pressure Ulcer Advisory Panel (NPUAP).

The majority of respondents stated that they did not have national registries for PU, but that they registered similar data on a local level (tab. 3).
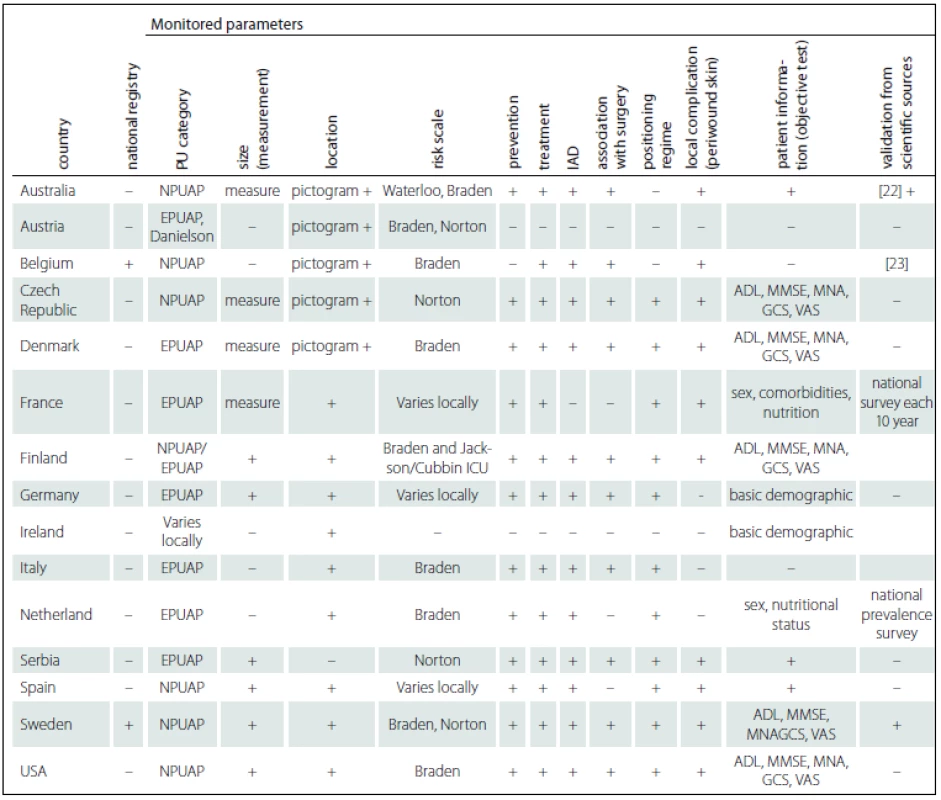
It was clear from the questionnaire responses that there were diverse situations concerning PU monitoring even within the countries. We thus decided to present one specific registry operating on the national level in Sweden.
The Swedish National Quality Registry of Ulcer Treatment
Solid clinical patient-oriented research within the framework of RUT has shown that through use of the registry a quality-assured treatment for these patients can be achieved, with reduction of healing times, antibiotic treatment, and costs as well as improved quality of life [5,6,10]. Data from RUT show how structured and uniform collection of data on a national level could be used to illustrate evidence-based practices.
Reduction of healing time
A significant reduction of ulcer healing time was seen for patients registered in RUT, from 146 days in 2009 to 53 days in 2015 [5].
Reduction of antibiotic treatment
Considering all years between 2009 and 2012, antibiotic treatment for patients with hard-to-heal ulcers was reduced from 71% before registration to 29% after registration of ulcer healing [5]. Today, overall antibiotic treatment lies within 26% except for diabetic foot ulcers with 42% in 2014 (unpublished data).
Reduction of per-patient costs
A recently published study from RUT showed a significant reduction of average costs per patient with healed ulcers, regardless of diagnosis, from €4,168 in 2009 to €2,235 in 2012 (a decrease of 46%). The results showed that staff costs accounted for 87% of total costs and the cost of dressing material for the remaining 13%. The reduction in treatment costs was seen as a direct consequence of the patients’ receiving adequate diagnosis and hence effective treatment [10].
Pressure ulcers in RUT
Patients with PU registered in RUT constitute 12% of all ulcers. These patients have a mean age of 75 years compared with 79 years for patients with other ulcer aetiologies, and the majority (53%) are men, compared with 42% for other ulcer patients. For patients with PU registered in RUT, there was a reduction of healing time from 153 days in 2009 to 91 days in 2014.
Discussion
In this study, we found that there was very limited interest in answering a survey on national registries on patients with PU, even when reaching out to international organisations for ulcer patients such as EWMA and EPUAP. This could be explained by two facts: the complex situation of patients with PU, and the lack of robust national data. Many research projects have focused on patients with PU [11 – 13], but most of this research has been carried out in smaller studies which did not grasp the whole situation of patients with PU. The task of capturing the entire complex clinical picture of PU patients is challenging both on the national and the international level [8,14].
Since PU are one of the most common injuries caused by health care [8], they should attract more scientific interest from researchers. Patients of all ages and conditions can be affected; the acutely ill as well as the chronically or terminally ill [15,16]. One large group is younger patients using wheelchairs. About 15% of patients in emergency hospitals have at least one PU [8].
Data such as those from an international study conducted by the Czech Republic show that a variety of risk assessment scales for PU identification and measurement are used, which makes it difficult to compare data on an international level or even within some countries (tab. 3).
National data have long been used in Sweden [17,18], where around 100 national quality registries have been established in recent decades with the aim of gathering data on diagnoses, symptoms, interventions, and treatment outcomes for a continuous systematic evaluation of medical practice.
In the Czech Republic, efforts have been made to present the incidence and prevalence of PU, but the lack of national standards and clinical guidelines has severely impaired every investigation. PU are registered in two databases, the National System for Reporting Adverse Events (NSRAE) and the National Register of Hospitalized Patients (NRHOSP). NSRAE serves as voluntary feedback on the quality of health care provided, while NRHOSP registers inpatients whose hospitalization ended during the observed period; PU are identified on the basis of the hospitalization diagnosis according to the 10th revision of the International Classification of Diseases (ICD-10). The intention is that every patient with the diagnosis code L89 is recorded, but this often has not happened in practice, as some patients, especially those with lower categories of PU, did not receive PU as their official medical condition. According to information obtained from previous research based on adverse events, the prevalence of PU was 1.86% in surgical sites, 4.53% in internal departments, 10.89% in intensive care units and 12.87% in aftercare (long-term care) wards [19–21].
Given the above information, it is difficult to compare our data with results from earlier research, due to uncertainty in registering and inconsistency in reporting data. We further find it necessary to use existing e-health solutions like Telemedicine and RUT’s bedside application, which was developed to allow initial registration to be made using a smartphone. Data in some Swedish national quality registries can be easily transferred from the patient’s medical record to the registry, and in the near future this will also be the case for RUT. This would facilitate the establishment of a true network for clinicians and researchers, for the benefit of all those with PU.
Conclusion
A lack of national data seriously impairs efforts to develop an international research network on patients with PU and to share data and expert knowledge and skills. Although existing data from quality registries on PU prevention are scarce and inconsistent, the task of establishing a common minimum data set in an international setting seems worthwhile. The minimum data set of the Swedish National Quality Registry on Ulcer Treatment, along with the new electronic tool for PU monitoring developed in the Czech Republic, could be used in such a setting in order to find new ways to prevent, treat, and facilitate the lives of people with PU and those who are at risk of getting one.
This study was supported by the Ministry of Health of the Czech Republic, grant no. 15-29111A with the title “The register of decubitus ulcers – integration strategy for monitoring and preventive interventions on the national level”. All rights reserved.
The authors declare they have no potential conflicts of interest concerning drugs, products, or services used in the study.
The Editorial Board declares that the manuscript met the ICMJE “uniform requirements” for biomedical papers.
assoc. prof. dr. Andrea Pokorná, Ph.D.
Department of Nursing
Faculty of Medicine
Masaryk University
Kamenice 5
625 00 Brno
e-mail: apokorna@med.muni.cz
Accepted for review: 27. 5. 2016
Accepted for print: 14. 6. 2016
Zdroje
1. Whitfield MD, Kaltenthaler EC, Akehurst RL, et al. How effective are prevention strategies in reducing the prevalence of pressure ulcers? J Wound Care 2000;9(6):261 – 6.
2. Kaltenthaler E, Whitfield MD, Walters SJ, et al. UK, USA and Canada: how do their pressure ulcer prevalence and incidence data compare? J Wound Care 2001;10(1):530 – 5.
3. International guidelines. Pressure ulcer prevention: prevalence and incidence in context. A consensus document. London: MEP Ltd 2009.
4. Padula W, Mishra MK, Makic MB, et al. Improving the quality of pressure ulcer care with prevention, a cost effectiveness analysis. Medical Care 2011;49(4):385 – 9. doi: 10.1097/ MLR.0b013e31820292b3.
5. Öien RF, Forssell H. Ulcer healing time and antibiotic treatment before and after the introduction of the Registry of Ulcer Treatment – an improvement project in a national quality registry in Sweden. BMJ Open 2013;3(8):e003091. doi: 10.1136/ bmjopen - 2013-003091.
6. Öien RF, Åkesson N, Forssell H. Assessing quality of life in patients with hard-to-heal ulcers using the EQ-5D questionnaire. J Wound Care 2013;22(8):442 – 7.
7. Hopkins A, Dealey C, Bale S, et al. Patient stories of living with a pressure ulcer. J Adv Nurs 2006;56(4):345 – 53.
8. SBU. Chronic ulcers in the elderly – prevention and treatment. Stockholm: Swedish Council on Health Technology Assessment (SBU) 2014. SBU report no. 226 (in Swedish).
9. Moore Z, Cowman S. Pressure ulcer prevalence and prevention practices in care of the older person in the Republic of Ireland. J Clin Nurs 2012;21(3 – 4):362 – 7. doi: 10.1111/ j.1365-2702.2011.03749.x.
10. Öien RF, Forssell H, Ragnarson Tennvall G. Cost consequences due to reduced ulcer healing times – analyses based on the Swedish Registry of Ulcer Treatment. Int Wound J 2015 in press. doi: 10.1111/ iwj.12465.
11. Orsted HL, Rosenthal S, Woodbury MG. Pressure ulcer awareness and prevention program: a quality improvement program through the Canadian Association of Wound Care. J Wound Ostomy Continence Nurs 2009;36(2):178 – 83. doi: 10.1097/ 01.WON.0000347659. 79722.b0.
12. Sanada H, Miyachi Y, Ohura T, et al. The Japanese Pressure Ulcer Surveillance Study: a retrospective cohort study to determine prevalence of pressure ulcers in Japanese hospitals. Wounds 2008;20(6):176 – 82.
13. Lindholm C, Sterner E, Romanelli M, et al. Hip fractureand pressure ulcers – The Pan-European PressureUlcer Study – intrinsic and extrinsic factors. Int Wound J2008;5(2):315 – 28. doi: 10.1111/ j.1742-481X.2008.00452.x.
14. National Pressure Ulcer Advisory Panel, European Pressure Ulcer Advisory Panel and Pan Pacific Pressure Injury Alliance. Prevention and Treatment of Pressure Ulcers: Quick Reference Guide. Haesler E, ed. Cambridge Media: Osborne Park, Western Australia 2014.
15. VanGilder C, Amlung S, Harrison P, et al. Results of the 2008 – 2009 International Pressure Ulcer Prevalence Survey and a 3-year, acute care, unit-specific analysis. Ostomy Wound Manage 2009;55(11):39 – 45.
16. Thomas DR, Compton GA. Pressure Ulcers in the Aging Population: a Guide for Clinicians, Aging Medicine 1. New York: Springer Science + Business Media 2014.
17. Zethelius B, Gudbjörnsdottir S, Eliasson B, et al. Level of physical activity associated with risk of cardiovascular diseases and mortality in patients with type-2 diabetes: report from the Swedish National Diabetes Register. Eur J Prev Cardiol 2014;21(2):244 – 51. doi: 10.1177/ 2047487313510893.
18. Andell P, Erlinge D, Smith JG, et al. ß-blocker use and mortality in COPD patients after myocardial infarction: a Swedish nationwide observational study. J Am Heart Assoc 2015;4(4):e001611. doi: 10.1161/ JAHA.114.001611.
19. Moore Z, Cowman S, Conroy RM. A randomized controlled clinical trial of repositioning, using the 30° tilt, for the prevention of pressure ulcers. J Clin Nurs 2011;20(17 – 18):2633 – 44. doi: 10.1111/ j.1365-2702.2011. 03736.x.
20. Müllerová N. Sledování dekubitů jako indikátorů kvality ošetřovatelské péče na národní úrovni. Tempus Medicorum 2011;20(7 – 8):18 – 24.
21. Kožený P. Sledování dekubitů jako indikátoru kvality ošetřovatelské péče. [online]. National Refrence Center, Prague, 2009. Available from URL: http:/ / www.nrc.cz/ aktualne/ nrc-v-mediich/ sledovani-dekubitu-jako-indikatoru-kvalityosetrovatelske - pece/ in Czech/ .
22. Gibb M, Chua XY, Gorse D, et al. The Australian wound registry. Aust Nurs Midwifery J 2015;23(3):35.
23. Health Belgium. [online]. Available from URL: http:/ / health.belgium.be/ internet2Prd/ groups/ public/ @public/ @dg2/ @healthprofessions/ documents/ ie2divers/ 19097134_nl.pdf.
Štítky
Dětská neurologie Neurochirurgie NeurologieČlánek vyšel v časopise
Česká a slovenská neurologie a neurochirurgie

2016 Číslo Supplementum1
-
Všechny články tohoto čísla
- The Relevance of Pressure Mapping System in Wheelchair Mobility
- International Cooperation in Pressure Ulcers Prevalence, Prevention and Treatment is Challenged by the Lack of National Registries
- The Importance and Limits of the Pressure Ulcer Surgical Debridement
- Incontinence-associated Dermatitis – Current Knowledge on Etiology, Diagnosis and Prevention
- Sorrorigens Wounds, Their Identification and Treatment Process
- Decubitus as a Cause of Death even in the 21st Century
- Evaluation of Selected Pressure Ulcer Management International Guidelines (AGREE II Tool)
- Implementation of Pressure Ulcer Prevention Guidelines – Where to Start?
- Editorial
- The Pressure Ulcers Monitoring in Patiens with Neurological Diseases – Analyse of the National Register of Hospitalized Patients
- Česká a slovenská neurologie a neurochirurgie
- Archiv čísel
- Aktuální číslo
- Informace o časopisu
Nejčtenější v tomto čísle
- Sorrorigens Wounds, Their Identification and Treatment Process
- Incontinence-associated Dermatitis – Current Knowledge on Etiology, Diagnosis and Prevention
- The Importance and Limits of the Pressure Ulcer Surgical Debridement
- The Relevance of Pressure Mapping System in Wheelchair Mobility
